In case of a dental emergency that requires same day bookings, please call 08 9276 1540
ROOT CANAL TREATMENT
From $1200*
If the pulp becomes infected or contaminated by decay, the tooth becomes painful and root canal treatment is usually indicated.
Depending on how the tooth will respond to the treatment, it usually takes between 3-5 visits with the final restoration.
*depending on tooth and number of visits
The dental pulp is the soft tissue inside the canal or channel that runs through the root of your tooth. The dental pulp consists mainly of blood vessels, tissue fibers and some nerve fibers. The main function of the dental pulp is to regulate the growth and development of the tooth during childhood. Once the tooth is fully formed, nutrition for the tooth comes from the tissues surrounding the root. Which means a tooth can function without its pulp (nerve) and, in the majority of cases, can be kept permanently. After root canal treatment the tooth is pulpless, but it is not a dead tooth.
The most common cause of pulp damage is deep tooth decay, which allows bacteria to reach the pulp. The pulp may then become inflamed or infected. Products of infection may then spread through the opening at the tip of the root into the surrounding bone – an abscess could result and this may cause pain and swelling. Other causes of pulp damage include: traumatic blows to teeth, leakage around old or loose fillings, excessive wear of teeth, and cracked teeth. These processes can also lead to the infection of the pulp.
By removing the infected pulp, cleaning and shaping the root canals, the dentist relieves inflammation and any discomfort. The root canals can then be filled and sealed. Afterwards, you return back to your dentist, who places a crown or other restoration over the remaining tooth to protect it. Once restored, the tooth continues to function like any other tooth.

Treatment
Root canal treatment is most often provided in a dental office setting. Before the procedure begins, local anesthesia (usually a numbing shot) is given so you won’t feel any pain. If you are especially nervous, your dentist may recommend an oral sedative or anti-anxiety medication. Be sure to mention your concerns in advance so you can discuss your options.
Next, the tooth under treatment will be isolated from the rest of the mouth by a thin sheet of rubber or vinyl called a “dental dam” to protect against bacterial contamination. Then, the endodontist will use a miniature drill to create access to the pulp chamber and root canal(s) either from the chewing surface of an affected back tooth, or from the backside of a front tooth.
Using specially designed instruments, the dentist will next remove all the diseased pulp tissue from the entire length of the root canal(s) and pulp chamber, and disinfect them with antiseptic and antibacterial solutions. Then, the dentist will shape the pulp chamber and canal(s) with tiny flexible instruments to optimize them for receiving filling and sealing materials. The cleaned space is typically filled with gutta-percha, a rubber-like natural material. The final step is the insertion of temporary or permanent filling material to seal the access hole that was made to treat the canal(s). After the procedure is finished, you will return home.
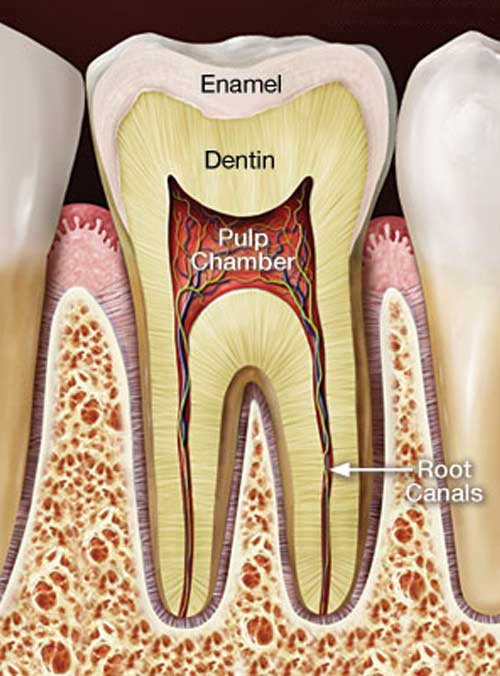
A cross section of a healthy tooth
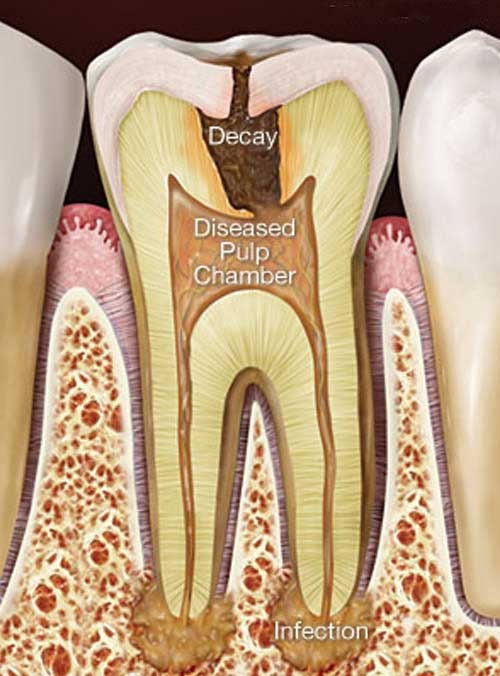
A cross section showing infection from tooth decay
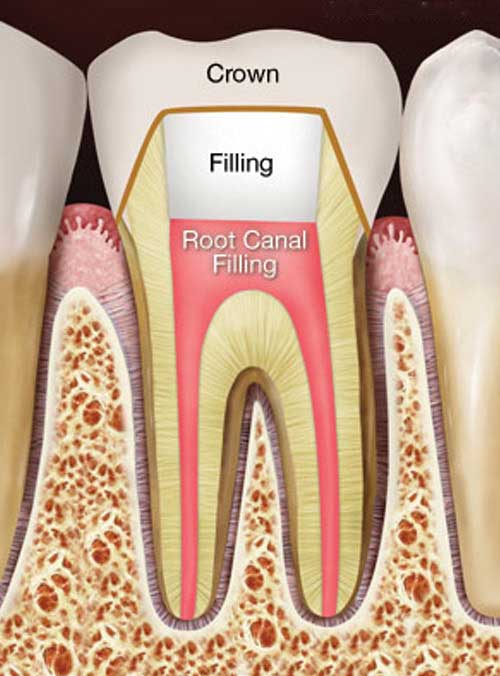
Completed root canal treatment and restoration
Smart Choice
REQUEST A CONSULTATION








